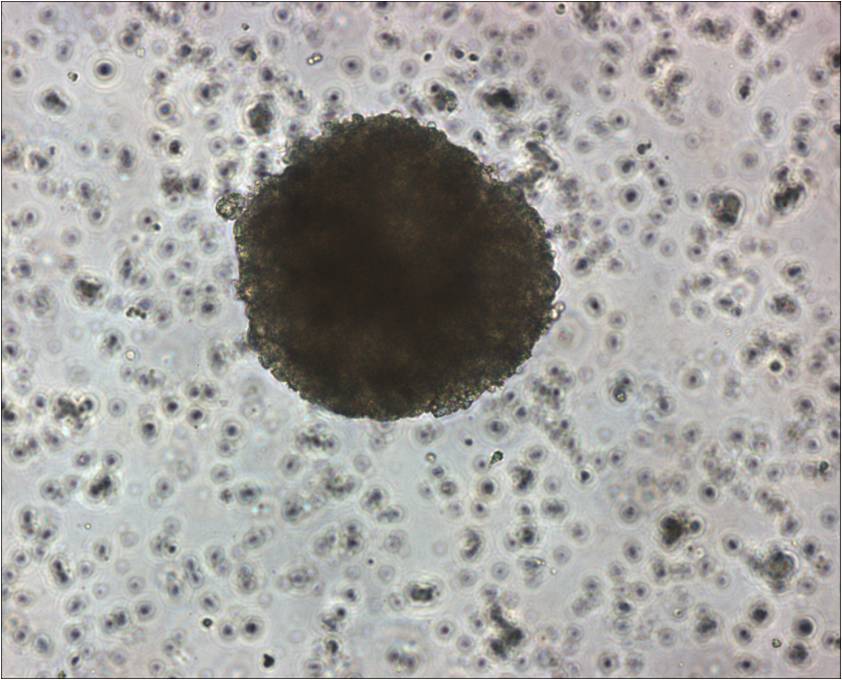
There are a number of types of stem cells including adult, embryonic and now induced pluripotent stem cells. Adult stem cells are the stem cells found throughout the body after birth that help regenerate tissue when one becomes hurt or regularly replaces cells as they become “old”. Adult stem cells include mesenchymal stem cells that can be found in bone marrow or neural stem cells that can be found in the subventricular zone of the brain. These stem cells hold significant promise as a cell therapy for a number of diseases; however they are not able to form all the cell types in the body limiting their potential.
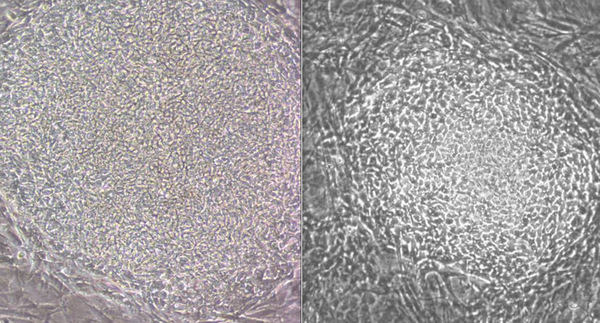
Embryonic stem cells (ESCs) are stem cells derived from the inner cell mass of developing embryos. These cells are pluripotent- meaning they can turn into any cell type in the body- making them an excellent candidate for cell therapy. Induced pluripotent stem cells (iPSCs) are a novel class of stem cells that, like their ESC counterpart, can turn into any cell type in the body. Yet, what makes these cells unique is the manner in which they are derived. iPSCs are generated by overexpressing a combination of six reprogramming genes (POU5F1, SOX2, NANOG, LIN28, KLF4 or C-MYC), eliminating the need for isolation of cells from developing embryos. Attempting to fulfill the promise of stem cells, both ESCs and iPSCs have shown great potential to turn into neural cells that can treat rodent models with neural degenerative diseases or develop into beta islet cells that can help diabetic mice. These tests in rodents clearly show the possibilities, yet the question remains how to safely take these findings and treatments from mice to people.

The potential of ESCs and iPSCs as a cell therapy for a number of diseases is still years away. However, these cells in many ways can make a significant contribution NOW as a cell source for toxicology or drug development screens. For example, many conditions are related to abnormal human sperm or egg development including reoccurring spontaneous abortions, infertility and Down’s syndrome. These conditions can often be linked to toxins. However it is challenging to screen the thousands of new compounds developed each year for toxic effects particularly because there is limited access to appropriate sperm, early sperm cells that can only be isolated directly from the testes and not through ejaculated sperm, or eggs. Stem cell derived germ cells could potentially fill this niche with stem cells being capable of generating billions of cells that can be used in this screening process. This approach can be easily adapted to hundreds of possible cell types that can be derived from stem cells to test for potential toxic effects in different tissues. Screening using human stem cell derived cells also has the added advantage of being human specific, eliminating the need to extrapolate results from mice or other model systems to humans. In addition, these cells may significantly decreasing the number of animals needed for testing potential toxins or new drugs- key factors of consideration when attempting to safely develop new chemicals and compounds.